Each year, approximately 80,000 Canadians are diagnosed with skin cancer each year? Of those, nearly 5,000 will be diagnosed with a form of melanoma skin cancer that will require some sort of surgery to remove it. With modern medical advancements, more treatments are available for skin cancer than ever, including a wide variety of surgeries. Before a patient decides if they want to pursue surgery, they should make sure they are well informed of their options. Keep reading to learn what kinds of surgery are available for skin cancer treatment, and what the associated risks are.
Mohs Surgery
One of the most commonly used and known surgical treatments is called Mohs Surgery. Mohs surgery is most effective when the cancerous cells are visible, making it a common option when removing skin cancer tumours. The technique involves the medical doctor removing the skin by layer until the cancer is no longer visible by examining each layer. While the process can be time-consuming, it has seen much success as a treatment, particularly for cancers that are prone to returning. In addition to its effectiveness, Mohs surgery is known to reduce the chances of significant scarring. Mohs surgery can be used for basal-, squamous and some types of melanomas, typically on the face, where it is important to preserve as much tissue as possible, like on lips, noses, and ears. Mohs surgery is unfortunately only available in Vancouver and Calgary with relative long waiting times.
Excision
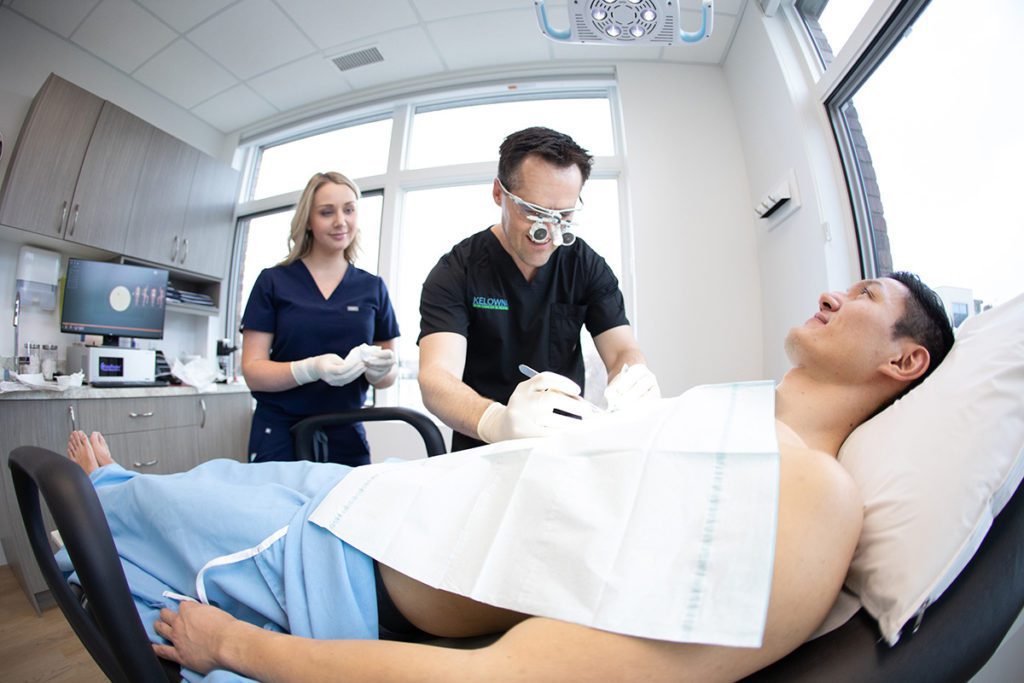
During an excision, the cancerous tumour is removed, in our office, by cutting it out of the body after the area is cleaned and numbed with freezing. Unlike Mohs surgery, which peels each layer back, Dr. Ben cuts into or around the tumour, removing it all at once. When a tumour is removed, a certain amount of normal tissue needs to come with the tumour, to make sure it does not come back. It is typical to add 2-10mm all around the tumour for removal. After the tumour is removed, the affected area is stitched up. The tumour is then sent to a pathologist at Kelowna General Hospital to tell us what cancer it is and if we got it all. If the pathologist reports that we did not get it all, we will have to remove a bigger piece. While the surgery typically leaves a scar, its size will depend on the size of the tumour, its location, and how advanced the cancer is. The scar will be larger than the tumour, due to the “extra normal skin” that was removed with the tumour.
Curettage and Electrodesiccation
Those who are diagnosed with superficial basal cell carcinoma or squamous cell carcinoma may be recommended for curettage and electrodesiccation. Using an approach that scrapes the cancerous tumour off of the skin, the medical doctor then moves on to treat the area with an electric needle. Because of its process, patients with more advanced forms of skin cancer should avoid this treatment. Scaring is also a big side effect from this form of treatment.
Laser Surgery
Laser surgery is another option for skin cancers that did not spread and remained on the superficial surface. The surgery involves using a strong, focused laser beam to break down the cancerous cells on the patient’s skin. We don’t make use of laser surgery at Kelowna Skin Cancer Screening clinic.
Lymph Node Removal
For patients who were diagnosed with a form of melanoma skin cancer, a lymph node surgery (biopsy), may be recommended when a more aggressive approach is needed. This is usually done by a general surgeon in the hospital, who will take specific lymph node/s out of the patient’s body to examine for cancerous cells, which can help determine if cancer has spread. If they find that cancer has spread (metastasized), this will help to determine the course of action related to treatment, working with your cancer doctor (oncologist).